Cell engineering is a rapidly evolving technology to treat diseases by controlling and directing cellular networks in the body. Whereas gene therapy seeks to alter the genetic makeup of cells, cell engineering goes a step further to consider how cells interact and ultimately function.
Cell engineering is based on understanding how cells function in the body and how to alter these functions to achieve therapeutic success. Cells communicate with each other in response to changes in their environment. Cells receive signals from other cells and transmit another signal to other cells to achieve specific biological functions. Cell engineering controls this process by providing molecular tools that direct the input cells receive, leading to a desired output.
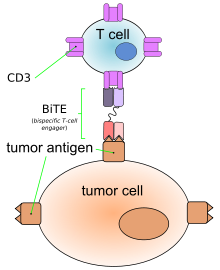
CAR T cell technology is an example of cell engineering developed as a customized response to treat cancer. The patient’s own cells are genetically modified to produce a specialized receptor on its surface. The engineered T cells are thereby reactivated to attack cancer cells.
Cell engineering can also be applied to multicellular networks to achieve tissue remodeling and regeneration of tissues. Potential applications of cell engineering include controlling autoimmunity, inflammation, regeneration and repair of tissues, and even synthesis of new organs.
Engineered cell therapies offer advantages over currently used molecular therapies, such as biologics or drugs. They can be less toxic as they are more targeted in action and do not interfere with other biological functions. Cell therapies can also aid in homeostasis or balance in body functions.
In addition to cancer, cell therapies could benefit other therapeutic areas. In cases of autoimmunity or inflammation, the goal is suppression. In the regeneration or repair of injury sites, cell therapies could induce targeting, cell differentiation, and blood vessel growth at the injury site.
REFERENCES
Lim, Wendell. “The emerging era of cell engineering: Harnessing the modularity of cells to program complex biological function.” Science. 378;6662; 848-851.